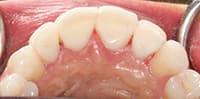
Quite often, dentists are the first health professionals to recognize the effects of bulimia nervosa. As dentists, we all know how much havoc bulimia can wreak on the health of a person’s teeth. Worn, ragged, chipped, thin, weak, and fragile are just a few of the words that are used to describe the irreversible damage that bulimia can cause to teeth (Figure 1). As a result, a person can have pain, increased tooth decay, gingival recession, xerostomia, an unattractive smile, decreased self-esteem, as well as oral pain that can significantly affect the patient’s quality of life. In severe cases, full-coverage crowns may be the only option. In an effort to help these patients, full-coverage restorations require even more tooth removal (especially on the facial and interproximal surfaces), further reducing any remaining sound tooth structure, making the teeth more fragile. This can make the patient even more self-conscious. If treated and restored early, before the damage is too severe, crowns, and all that they entail, can be avoided in these patients.
AN ALTERNATIVE APPROACH
So, if full-coverage crowns are not always the optimal treatment for lingual incisal acid-eroded teeth, what is? Rather than removing any healthy enamel from the facial and interproximal surfaces, lingual veneers coupled with cosmetic facial bonding, offer a conservative alternative. The goals are to build up and restore worn-away teeth, while preserving as much of the natural tooth structure as possible. Lingual veneers should be considered whenever possible. The more tooth structure that we can save and “bank” for later, the better.
CASE REPORT
Diagnosis and Treatment Planning
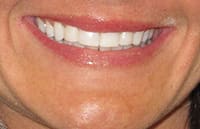
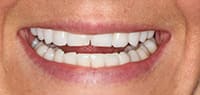
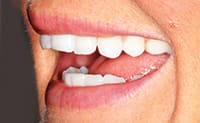
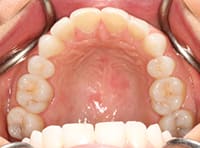
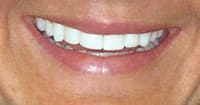
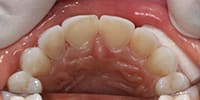
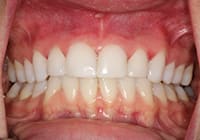
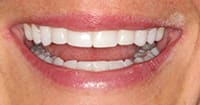
A 25-year-old female patient presented with severe sensitivity due to the extensive loss of enamel on the inside of her front teeth as a result of an eating disorder. She was also very self-conscious about her looks (Figure 2). The fragile edges of the upper front teeth gave the patient an inverted, negative smile, and a worn-out appearance with noticeable, transparent, or “see-through” edges (Figure 3). The upper centrals exhibited advanced enamel loss extending from the back sides, beyond the incisal edges, all the way to the front surfaces, causing severe sensitivity when eating or drinking (Figure 4). The profile view (Figure 5) shows the reverse smile-line that negatively affected her self-confidence and appearance, and compromised her dental health. This caused her even further stress. On the lingual surfaces, erosive wear from the acid was evident, a typical presentation in bulimia cases, resulting in enamel loss and painful teeth (Figure 6). Since she had consulted with several dentists before arriving in our office, she was well versed on what “conventional dentistry” could do to improve her condition. All of the doctors had recommended treatment plans calling for an array of different types of crowns. However, she did not want this. After countless hours of research, and a healthy determination to keep her own teeth, she arrived at our office in Dallas hopeful that there was another solution to her dental dilemma. When she heard that lingual veneers would be a viable option for her, she was greatly relieved. This was what she was looking for. In less than 15 minutes, we showed her a SEZI (SmilePix) cosmetic image of her existing smile simulating what her final outcome would look like. Her treatment would consist of a combination of lingual veneers and cosmetic bonding on the facial surfaces to lengthen her upper incisors (Figure 7).
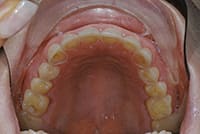
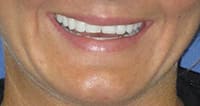
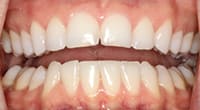 Figure 3. A close-up of the patient’s smile shows fragile edges of the upper front teeth that gave
Figure 3. A close-up of the patient’s smile shows fragile edges of the upper front teeth that gavethe patient an inverted smile and a worn-out appearance with noticeable, see-through edges.
She loved the aesthetic value of the lingual veneers, but more importantly, the patient appreciated the conservative nature of the treatment, saving the rest of her teeth.
Clinical Protocol
Due to severe sensitivity (even to air), Septocaine (Septodont) was buffered by OnSet (Onpharma) at the chair, and administered with The Wand (Aseptico) for a painless injection that would also provide rapid onset. As a more conservative treatment, lingual veneers demand careful planning and contouring of the teeth to ensure preservation of as much healthy natural tooth structure as possible. A smooth, football-shaped diamond (NTI 80456 [Axis Dental]) and small round burs were used to smooth the sharp corners of enamel and create a definitive finish line. The final preps should be very minimal, yet allow (0.5 mm) for sufficient thickness and a positive seat of the lingual veneers (Figure 8). Preservation of healthy tooth structure provides strength and reinforcement while drastically reducing postoperative sensitivity so that a healthy diet and lifestyle can be resumed. A vinyl polysiloxane (VPS) (Impressiv [Cosmedent]) upper impression and a VPS bite registration (Blu-Mousse [Parkell]) were taken. Temporization was done using simply 2 applications of Tokuyama Varnish over the prepared surfaces and, as a result, she reported less interim sensitivity than before the preparations.
The indirect composite lingual veneers were fabricated (Pearlfect Smile Veneer [Mizrachi Dental Lab]) using an indirect composite (Premise Indirect [Kerr]) that is processed in a nitrogen environment under pressure, providing 100% conversion of the monomer as compared to 70% with just light-curing alone. Figure 9 shows the final restorations from the lingual perspective on the lab casts. From the front view, the upper front teeth have been restored to their original length with the lingual veneers extending to the incisal edges and onto the facial surface (Figure 10). This is an additive process—tooth augmentation, rather than amputation.


The bonding protocol was the same as if placing facial veneers. Prevue (Cosmedent) try-in pastes were used to accurately select the correct cement shade. Anesthesia was administered (as described above), and the teeth were isolated using metal strips. The teeth structure to be bonded to was sandblasted (EtchMaster [Groman]) to increase the surface area for greater retention and bond strength. We then used a total-etch bonding technique to seat the lingual veneers with a resin cement system (Complete adhesive and Insure cement [Cosmedent]).
Once bonded, a “sandwich” bonding technique was utilized. With the lingual veneers as a matrix adding length and strength from the back side, a microfill composite resin (SB3 Renamel [Cosmedent]) was placed and sculpted on the facial surfaces to build up and improve the aesthetics (Figure 11). Nano/microhybrid diamond polishes, discs (FlexiDiscs [Cosmedent]), and Enamelize (Cosmedent) polishing paste finished the restorations. The patient’s full smile shows how the worn edges were elongated and evened out to create a beautiful and proportional smile (Figure 12). The lingual sandwich veneers strengthened and reinforced the teeth from further damage and drastically reduced sensitivity so a healthy diet and lifestyle could be resumed (Figure 13). These conservative restorations not only restored the patient’s dental health and her beautiful smile, but they also succeeded in revitalizing her appearance and self-confidence (Figure 14).
Figure 13. Palatal view immediately after veneers were placed. The lingual veneers replaced the lost enamel while protecting the tooth from further acid erosion.
Figure 14. The lingual sandwich veneers successfully restored the patient’s dental health, appearance, and self-confidence.
CLOSING COMMENTS
Though dental practitioners are often the first healthcare providers to identify the erosive effects of bulimia nervosa, we may often be the last ones to address this condition with our patients. According to a recent article published in the April 2014 issue of the Journal of the American Dental Association, less than half of oral health professionals routinely evaluate patients for dental signs of eating disorders. It is up to our profession to become properly trained to approach this sensitive topic with patients who have suspected cases of bulimia so that we can then acknowledge, educate, and empower them to seek the proper care they so desperately need. By utilizing the latest and greatest techniques and materials available, we can help these patients regain optimal dental health, renewed confidence, a pain-free smile, and an improved quality of life. Remember, it all starts with a conversation.
Suggested Readings
Christensen GJ. Oral care for patients with bulimia. J Am Dent Assoc. 2002;133:1689-1691.
Conviser JH, Fisher SD, Mitchell KB. Oral care behavior after purging in a sample of women with bulimia nervosa. J Am Dent Assoc. 2014;145:352-354.
Debate RD, Tedesco LA. Increasing dentists’ capacity for secondary prevention of eating disorders: identification of training, network, and professional contingencies. J Dent Educ. 2006;70:1066-1075.
Valena V, Young WG. Dental erosion patterns from intrinsic acid regurgitation and vomiting. Aust Dent J. 2002;47:106-115.